What is Endometriosis?
Authors:
Vaishnavi Purusothaman, MD
Maddie Cheong
Medically Reviewed by Dr. Vaishnavi Purusothaman, Ob-Gyn
What is endometriosis and how common is endometriosis?
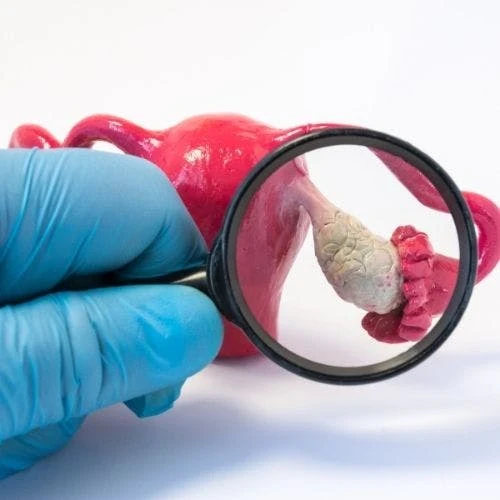
Endometriosis is a disorder where the tissue that is similar to the tissue lining the uterus, known as the endometrium, is found in places outside the uterus. Some common places that endometriosis implants can be found are the fallopian tubes, the ovaries, the bladder, and the colon (1). Endometriosis on the ovary is called an endometrioma, which is a fibrous cyst filled with old blood, similar to a “blood blister” (2). Endometriosis affects approximately 10% of women and is most commonly diagnosed between 30 to 40 years of age (1).
How do you get endometriosis?
Endometriosis is more common in some women than others. Women with a first- degree relative with a history of endometriosis or infertility are more likely to have endometriosis. Additionally, women giving birth for the first time after the age of 30 are also at greater risk of developing endometriosis (2). Menstrual cycles also play an important role in indicating the potential presence of endometriosis. Women experiencing short cycles (less than 27 days between periods) or unusually heavy cycles that last more than 7 days are also at a greater risk of having endometriosis (3).
How do you know if you have endometriosis?
Symptoms of endometriosis are often concentrated in the pelvis, and can include pain during your period, pain during or after sex, and pain during bowel movements or urination. There are many ways in which endometriosis can cause pain. Just like the endometrium found in the uterus, endometriosis tissue found in other areas can also bleed once a month, causing inflammation and pain. Another reason for the pain may be due to endometriosis lesions pressing against nerve cells, relaying pain signals to the brain. Finally, it is also possible that chemicals released by the endometriosis lesions may cause pelvic organs to stick to each other and create scar tissue, which can also cause pain. However, it is important to note that the size or number of endometriosis lesions in the pelvis do not correlate with the severity of pain (4). Moreover, not all women with endometriosis will display symptoms: approximately 25% of women with endometriosis are asymptomatic (5).
Can you get pregnant with endometriosis?
Related: Is My Vagina Normal? Plus A Female Anatomy Chart
About 40% of women with endometriosis experience infertility (1). Women with infertility are 6-8 times more likely to have endometriosis, and 30-50% of women with infertility have endometriosis (5). Endometriosis likely affects fertility through many mechanisms. Endometriosis on the ovary (also known as an endometrioma) has been shown to affect egg production and ovulation. Additionally, the inflammatory environment produced by endometriosis lesions has been shown to affect the quality and function of eggs, sperm, and embryos. Transport of the gametes (egg and sperm) is also affected by this inflammatory environment. The inflammation can alter motility in the fallopian tube and the uterus, which affects both fertilization of the egg and embryo implantation. Finally, endometriosis is thought to potentially alter the uterine lining by making it less receptive for an embryo to implant (6).
How to treat endometriosis?
Treatment of endometriosis often depends on the severity and frequency of symptoms. Mild symptoms can often be treated with over the counter pain medications, such as ibuprofen, that work to combat the inflammation caused by endometriosis. Another option is hormonal birth control, which can work to quiet the endometriosis lesions and make them inactive. There are also injectable and oral medications known as gonadotropin-releasing hormone (GnRH) agonists and antagonists that have been shown to alleviate pain. While these GnRH based treatments are very effective, they can be associated with side effects including hot flushes, vaginal dryness, and decreased bone density. These effects can be mitigated by using add-back hormonal therapy and using shorter durations of treatment (7).
Surgery is also an option for management of endometriosis. Surgical options can range from minimally invasive laparoscopic surgery to remove endometriosis lesions/implants to open abdominal surgery to do the same. Definitive surgical treatment of endometriosis involves removal of the uterus, fallopian tubes, and ovaries, and is used to treat patients with severe endometriosis who have not responded to other therapies (2). However, surgical treatments do not guarantee patients a complete eradication of symptoms; about 15% of women experience a recurrence of endometriosis related symptoms even after definitive surgical treatment (7).
References
- American College of Obstetricians and Gynecologists [Internet]. Washington D.C.: c 2021 [cited 2021 Feb 26]. Endometriosis; [about 1 screen]. Available from: https://www.acog.org/en/Womens%20Health/FAQs/Endometriosis
- Johns Hopkins Medicine [Internet]. Baltimore: c 2021 [cited 2021 Feb 26]. Endometriosis; [about 5 screens]. Available from: https://www.hopkinsmedicine.org/health/conditions-and-diseases/endometriosis
- Eunice Kennedy Shriver National Institute of Child Health and Human Development [Internet]. Bethesda: U.S. Department of Health and Human Services; c 2021[cited 2021 Feb 26]. What are the risk factors for endometriosis?; [about 2 screens]. Available from: https://www.nichd.nih.gov/health/topics/endometri/conditioninfo/at-risk#f2
- Eunice Kennedy Shriver National Institute of Child Health and Human Development [Internet]. Bethesda: U.S. Department of Health and Human Services; c 2021[cited 2021 Feb 26]. What are the symptoms of endometriosis?; [about 2 screens]. Available from:
https://www.nichd.nih.gov/health/topics/endometri/conditioninfo/symptoms - Bulletti C, Coccia ME, Battistoni S, Borini A. Endometriosis and infertility. J Assist Reprod Genet. 2010 Aug;27(8):441-7. doi: 10.1007/s10815-010-9436-1. Epub 2010 Jun 25. PMID: 20574791; PMCID: PMC2941592.
- Macer ML, Taylor HS. Endometriosis and infertility: a review of the pathogenesis and treatment of endometriosis-associated infertility. Obstet Gynecol Clin North Am. 2012 Dec;39(4):535-49. doi: 10.1016/j.ogc.2012.10.002. PMID: 23182559; PMCID: PMC3538128.
- Practice bulletin no. 114: management of endometriosis. Obstet Gynecol. 2010 Jul;116(1):223-236. doi: 10.1097/AOG.0b013e3181e8b073. PMID: 20567196.
We discuss products we think are useful to people. If you buy something through our links, we may earn a commission. Remember to check with your personal physician to see if a product recommended is right for you.