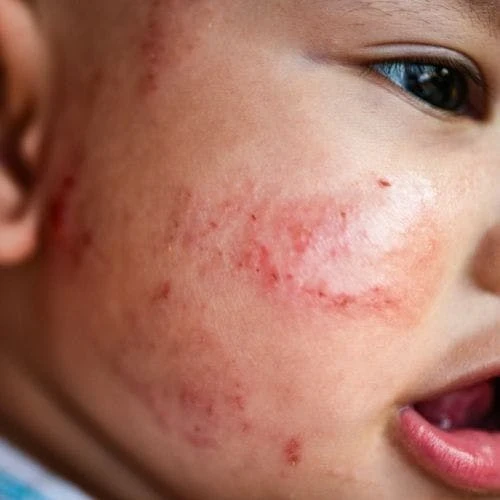
Signs Of Food Allergies In Babies
Your child ate something and is now neither looking nor feeling too good, but how can you tell if it’s a food allergy or simply a food intolerance? Because of the overlap of symptoms and lots of outdated and some misinformation out there, it is often hard to differentiate food allergies versus food intolerances.
Food Allergy Vs Food Intolerance?
Food allergies and food intolerances differ at the physiological level. A true food allergy is the result of your body creating an immune response (using an “antibody”) to the food you are eating (the target of the antibody, or the “antigen”). This is similar to a vaccine targeting a particular bacteria or virus. The type of antibody made is called IgE, and it is specific for a particular type of food. When it binds to that food, it releases something called histamine which ultimately leads to the symptoms of an allergic reaction and sometimes, anaphylaxis (a more severe allergic reaction) (2). Some IgE-mediated food allergies are outgrown in early childhood, and some stay for life (2). IgE to particular foods is something a doctor can measure through a blood or skin test.
Food Intolerance
Food intolerances are characterized by problems with your child’s digestion and/or digestive system (1). These are generally less severe and easier to treat, as many food intolerances can be treated by changing either the form of the food or what it is taken with to aid its digestion (1). For example, taking lactase pills before consuming lactose will likely allow an individual with lactose intolerance to consume lactose-containing items (1). Food intolerances are often referred to as “non-IgE mediated allergies”, although this term is misleading and confusing for parents. Unlike those with food allergies, individuals with food intolerance are not at risk for anaphylaxis (1).
What Causes Food Intolerance?
Some causes of food intolerance are unknown. Some food intolerances also may not last long, especially at a young age. There are some food intolerances that have an identifiable cause. These include:
- Absence of an enzyme needed to fully digest a food (1)
- Irritable bowel syndrome (1)
- Sensitivity to food additives that are used to enhance the preservation of foods (1)
- Recurring stress or psychological triggers (1)
- An allergic response that is limited to the gut – While classified as “allergic,” it is typically not IgE-mediated and does not lead to anaphylaxis
- Celiac disease – Although celiac disease concerns the immune system, people with this condition are not at risk of anaphylaxis so it is not classified as a food allergy (1).
Food Allergy Symptoms
Symptoms of food allergies can range from mild to severe. Since they induce an immune reaction that affects various organs in the body, the symptoms can be diverse (1). Some signs of food allergies include (3):
• Skin – Itching, flushing, hives (itchy, raised red bumps)
• Eyes – Redness or swelling
Related: Infant Eczema: Baby Skin Care And Baby Diaper Rash Care
• Nose and mouth – Sneezing, runny nose, nasal congestion, swelling of the lips or tongue
• Lungs or throat– Trouble breathing, wheezing, coughing
• Digestive system – Vomiting, diarrhea or pain leading to fussiness
• Other signs include – limpness, lethargy
Food Intolerance Symptoms
On the other hand, since food intolerance is more targeted to digestive system problems, symptoms are often (but not always) limited to vomiting, diarrhea, or abdominal pain (1). Some babies will develop constipation or gas with certain foods or even a change in stool pattern. These symptoms are often not consistent with an allergic reaction and you should discuss with your doctor to help determine if they are indeed allergic in nature.
Can A Mom Continue To Breastfeed If They Eat Foods Baby Is Allergic To?
In almost all cases, the answer is yes. Babies with food allergies and intolerances can continue to breastfeed. Generally, the mother does not need to remove the allergenic food from her diet prior to breastfeeding unless the baby is exhibiting immediate symptoms or if the baby is intolerant to cow’s milk protein (4). For babies that have cow’s milk protein intolerance, moms have to remove dairy from their diet, and in some cases soy, if they want to continue breastfeeding. Otherwise, they have to place the baby on a soy formula (if tolerated), a hydrolyzed formula that partially or fully breaks down the milk protein, or an elemental formula which does not contain any intact proteins. The good news is, most babies outgrow this intolerance by around one year of age! Currently, there are no official recommendations on other foods not to consume when breastfeeding when concerned about an allergy or intolerance, but research in that sector is constantly evolving (4). If you are concerned about your baby reacting adversely to your breast milk, it is best to consult with an allergist, who will help you determine the next best steps.
Allergy Testing On Baby
The most challenging part about feeding babies with concerning symptoms is determining what they are allergic to. Allergy testing can be done in babies but are often not reliable and need to be interpreted by an expert (4). Therefore, unless a specific food is identified that you are concerned about, specialists do not recommend a panel of allergy labs “just to see” if your baby has an allergy. This can lead to unnecessary elimination of foods from a child’s diet and can lead to nutritional deficits. Therefore, it is always recommended you see your pediatrician or allergist to discuss any concerns you may have with your baby’s diet and they can help you take the proper next steps.
Sources
- https://www.mayoclinic.org/diseases-conditions/food-allergy/expert-answers/food-allergy/faq-20058538
- https://www.chop.edu/conditions-diseases/ige-mediated-food-allergies
- https://www.uptodate.com/contents/food-allergy-symptoms-and-diagnosis-beyond-the-basics?topicRef=1185&source=see_link
- https://www.chop.edu/pages/breastfeeding-baby-food-allergies
We discuss products we think are useful to people. If you buy something through our links, we may earn a commission. Remember to check with your personal physician to see if a product recommended is right for you.