Treatment For Pelvic Floor Muscle Disorders & Dysfunction
Pelvic Floor Muscles & Anatomy
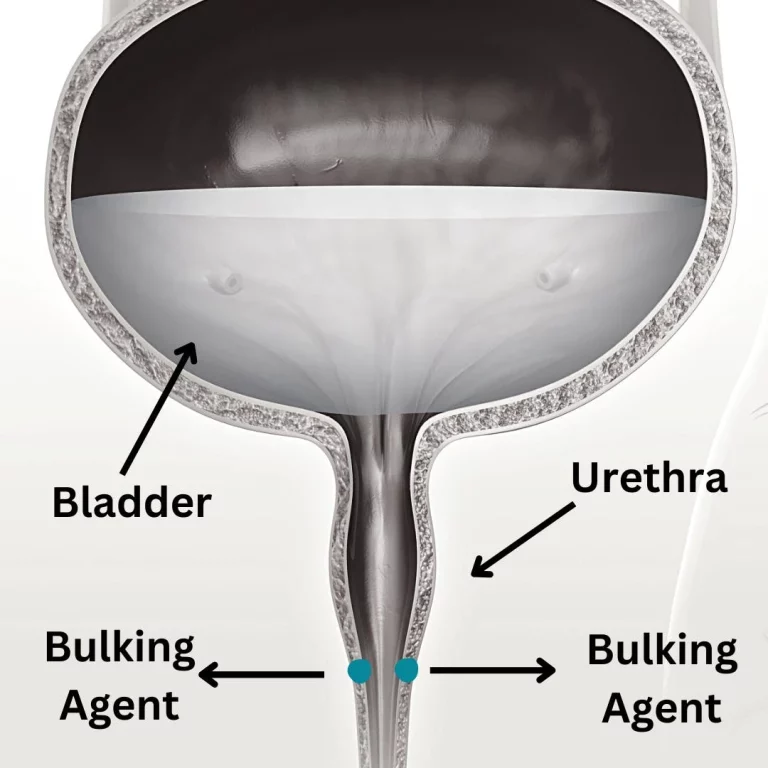
The pelvic floor muscles are a group of muscles that span the bottom of the pelvis, supporting the pelvic organs (bladder, uterus, and rectum) and helping to control the flow of urine and feces. These muscles of the pelvic floor form a sling-like structure that runs from the pubic bone at the front of the pelvis to the tailbone at the back. These muscles are responsible for maintaining continence, supporting the organs, and providing stability to the lower back and hips.
Symptoms Of Pelvic Floor Dysfunction
The pelvic floor muscles can become weakened or damaged due to factors such as pregnancy, childbirth, aging, obesity, chronic coughing, and straining during bowel movements. This can lead to problems such as urinary incontinence, pelvic organ prolapse, and sexual dysfunction.
Pregnant Women & Postpartum Period
Pelvic floor dysfunction is a common problem among postpartum women. Studies have shown that up to 50% of women experience some form of pelvic floor dysfunction after childbirth. This can include urinary incontinence, fecal incontinence, pelvic organ prolapse, and sexual dysfunction. The risk of developing pelvic floor dysfunction is higher among women who have had a difficult or prolonged labor, vaginal delivery with instrumentation (forceps or vacuum), or multiple births.
The duration of urinary incontinence after childbirth can vary from woman to woman, and it can depend on various factors such as the severity of the condition, the type of delivery, and individual healing rates. For most women, urinary incontinence after childbirth tends to improve within the first few weeks to months postpartum. However, for some women, it may take longer, and in some cases, it can persist for several months to a year or longer.
Studies have shown that up to 80% of women experience some form of urinary incontinence in the immediate postpartum period. Within 3-6 months postpartum, only about half of women report significant improvement in their urinary symptoms. For many women, this can be incredibly stressful, embarrassing and uncomfortable.
Exercises For Pelvic Floor Disorders
Physical therapy can be very helpful for improving pelvic floor dysfunction. There are physical therapists who specialize in the connective tissue that surrounds the pelvic muscles. A pelvic floor physical therapist however can be hard to make an appointment with and it may or may not be covered by insurance. Luckily you can try some exercises at home once you are cleared by your physician to do these exercises. Here are some exercises that can improve function of the pelvic muscles, as well as help with overactive bladder and bowel control.
Kegel Exercises
Kegel exercises are exercises that you can do at home that target the pelvic floor muscles. It’s important to avoid tensing your abdomen, buttocks, or thigh muscles while performing Kegels, as this can lead to improper muscle engagement. Also, make sure to breathe normally and avoid holding your breath while doing the exercises.
The pelvic floor muscles are the muscles that you use to stop the flow of urine or prevent passing gas. To identify these muscles, try stopping the flow of urine midstream. If you are able to do this, you have identified the correct muscles to do Kegels correctly. Once you have identified the correct muscles, empty your bladder and find a comfortable position to perform the exercises, such as sitting or lying down. Then, tighten your pelvic floor muscles as if you are trying to stop the flow of urine or prevent passing gas. Hold the contraction for 5-10 seconds, or as long as you can comfortably hold it. Finally, you can release the contraction and rest for a few seconds before repeating the exercise. Gradually increase the duration of the holds as your muscles become stronger. Repeat this several times a day, gradually increasing the duration of the holds.
There are medical devices that you can use that take the guess work out of doing kegel exercises correctly. This can be a huge advantage if you are short on time, as most postpartum women are, but still want to get your kegel exercises in. These devices can also help you do the exercises correctly so that you don’t have to struggle with leaking urine after pregnancy.
Squats
Squats involve the contraction and relaxation of the pelvic floor muscles to stabilize the pelvis and support the bladder, uterus, and rectum. They are usually a weight-bearing exercise that can help build strength in the muscles of the lower body, including the pelvic floor muscles. Squats can increase blood flow to the pelvic region, which can help promote healing and improve muscle function. When performed correctly, they can help improve flexibility and mobility in the pelvic area. Most importantly, squats also engage the core muscles, including the muscles of the pelvic floor, to provide stability and support to the lower back and pelvis.
Before beginning a squat, you can consider holding a five to fifteen pound weight depending on your strength. Stand with your feet shoulder-width apart and lower your body as if you are sitting down in a chair, keeping your weight in your heels. Repeat several times.
Pelvic Bridge
Related: How To Heal Perineal Scar Tissue After Childbirth
Bridges are another exercise that can help to strengthen the pelvic floor muscles, as well as the lower back and glutes. Lie on your back with your knees bent and feet flat on the floor. Lift your hips up towards the ceiling, hold for a few seconds, and then lower back down. Repeat several times.
A pelvic bridges can help to reset your pelvis and remind your body to use the hip and buttock muscles. It can also help to stabilize core muscle which also can be helpful with pelvic floor dysfunction since all the tissues and ligaments are connected. Additionally, a pelvic bridge is a safe option for patients who can not do squats due to knee pain or other join issues.
Yoga
Certain yoga poses can be helpful for improving pelvic floor function. Poses such as the Bridge pose, Cat-Cow pose, and Child’s pose can help to stretch and strengthen the pelvic floor muscles.
Activity Modification For Pelvic Floor Disorders
If you have stress incontinence, which is the leakage of urine when you cough, sneeze, laugh, or engage in physical activity, there are certain activities you may want to avoid or modify to reduce symptoms. Here are some examples:
- High-impact exercises: High-impact activities, such as running, jumping, or aerobics, can put extra pressure on the bladder and pelvic floor muscles, leading to urine leakage. Consider switching to low-impact exercises, such as walking, cycling, or swimming.
- Heavy lifting: Lifting heavy objects can also put extra strain on the pelvic floor muscles and increase the risk of urine leakage. Try to avoid heavy lifting or use proper lifting techniques, such as bending at the knees and lifting with your legs instead of your back.
- Caffeine and alcohol: Caffeine and alcohol can act as diuretics, increasing urine production and making it more difficult to control urine leakage. Try reducing your intake of these beverages or avoiding them altogether.
- Certain medications: Some medications, such as diuretics or blood pressure medications, can increase urine production and worsen stress incontinence. Talk to your healthcare provider if you are experiencing symptoms and are concerned about your medications.
- Constipation: Straining during bowel movements can put pressure on the pelvic floor muscles and worsen stress incontinence. Make sure to eat a diet high in fiber, stay hydrated, and try to establish regular bowel habits to reduce the risk of constipation.
Devices That Help To Treat Pelvic Floor Dysfunction
Elvie
The Elvie Pelvic Trainer is a device designed to help women strengthen their pelvic floor muscles. It consists of a small, egg-shaped device that is inserted into the vagina and connects to an app on your smartphone or tablet via Bluetooth. The app guides you through a series of pelvic floor exercises and provides real-time feedback on your muscle activity.
The Elvie Pelvic Trainer measures the strength of your pelvic floor contractions and provides feedback through visual cues on the app. The device is designed to be discreet and comfortable, and it can be used at home or on-the-go.
Yarlap
The Yarlap Pelvic Exercise Device is a medical device designed to help women strengthen their pelvic floor muscles. It is a small, handheld device that uses mild electrical stimulation to contract and relax the pelvic floor muscles, similar to a Kegel exercise.
The Yarlap device is designed to be easy to use and comes with pre-set programs for different levels of intensity and duration. It also has a patented AutoKegel® technology that adjusts the intensity of the electrical stimulation based on the strength of your pelvic floor muscles.
It’s important to talk to your healthcare provider if you are experiencing stress incontinence or other symptoms of pelvic floor dysfunction. They can evaluate your symptoms and provide guidance on treatments and lifestyle modifications that can help improve your bladder control.
Treatment For Pelvic Floor Muscle Disorders & Dysfunction: Summary
Pelvic floor dysfunction can be very difficult to deal with and can cause urinary incontinence as well as bowel incontinence. There are exercises and devices that can help to improve the function of your pelvic muscles. A pelvic floor physical therapist can also be very helpful and may be able to help virtually or in person.
We discuss products we think are useful to people. If you buy something through our links, we may earn a commission. Remember to check with your personal physician to see if a product recommended is right for you.